 Could in-house Facility Epidemiology manage healthcare $compensation costs?
Could in-house Facility Epidemiology manage healthcare $compensation costs?
David Huer, Vancouver, Canada.
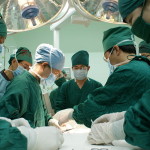
In Health Care as in all public safety and assurance occupations, it is vital to protect the trained caregiver from inadvertent harm because that person’s loss damages society’s ability to serve everyone.
I’ve been at home with flu for a week. Friends from the States came to visit throughout the Lower Mainland and up the coast, then we had a visit. Shortly thereafter, I got walloped. And then, whilst talking to them on the phone later, learned that a group of students, coughing and sniffly, came onto their connecting flight. And learned from my family physician that flu symptoms do not show for 12 hours after exposure. Making us suspect they might be the source vector.
Periodically, I volunteer business services to health clinics, and it was in thinking about that, and the vectoring of this flu, that I’ve been wondering:
Could we recognize a role for Transmitted Infection Vector (TIV) in $compensation rates at a healthcare facility?
Could we alter our definition of effectiveness in patient-centred care, to one where Health Worker salary $compensation is weighted to account for exposure to Patient Transmitted Infection (PTI). Recognizing the likelihood that the worker could become a Transmitted Infection Vector (TIV)?
- Identifying different risks of exposure of different classes of health worker?
- Recognizing that different classes have different risk to become TI Vector transmitters?
- Could this become the means to improve $compensation package effectiveness?
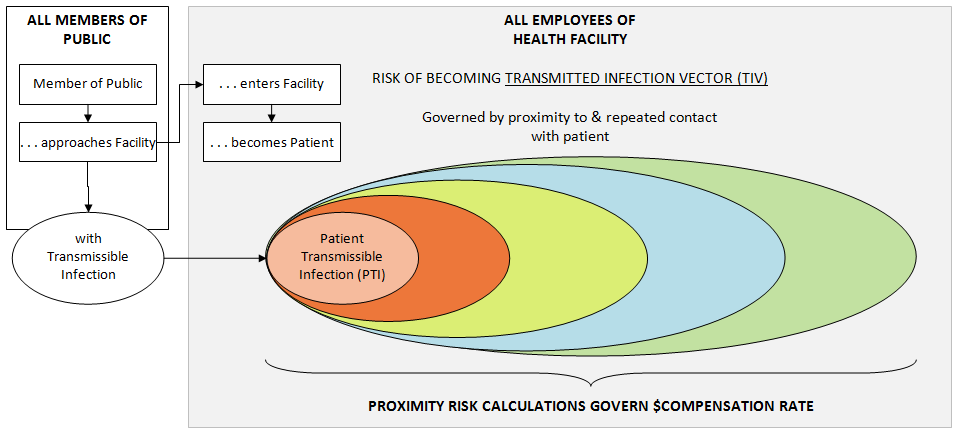
TIV Proximity Risk
WHERE TO START
Dartmouth’s Chris Trimble neatly summarizes healthcare innovation pathways at the Dec 2015 article here: http://www.kevinmd.com/blog/2015/12/innovation-health-care-delivery-can-boiled-4-ideas.html
- Standardize and delegate
- Coordinate
- Prevent
- Improve treatment decisions
All 4 paths influence this idea, and gathering the data set is enormously challenging if collected with traditional paper and interviews. But, local WiFi/GPS (Smartphone, Geo-fenced In-House Smartphones, Active ID cards) and machine-learning – accessed through programs like Samsung’s Enterprise Alliance Program – offer a nearly automated data-gathering method, that could make this an effective, scalable process and tool for private, public, and mixed-model social enterprise health facilities.
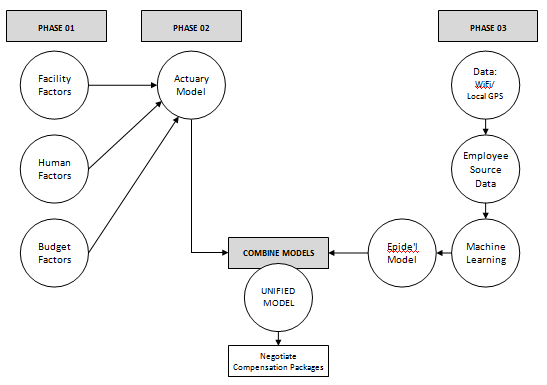
Building the Combined Model (Actuarial Model + Epidemiological Model) from source data
PHASE O1
- Determine Facility Factors
- Determine Human Factors
- Determine Budget Factors.
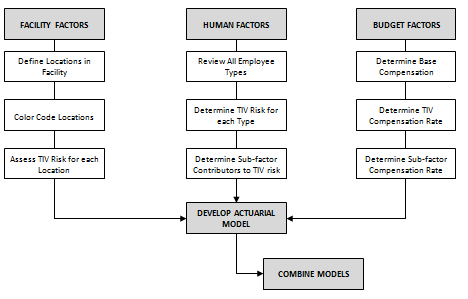
Building the Actuarial Model from source data
PHASE O2
- Build and test the Actuarial Model
PHASE 03
- Gather “employee path-taking data” to develop epidemiological data for analysis of likely TIV source-paths and source-points.
- Develop Epidemiological Model
SUMMARY PHASE
- Combine Actuarial and Epidemiological Models
- Negotiate $Compensation Packages
Example:
Using the University of New Mexico’s Dental Clinic and Surgery Center.
Rough calculations look interesting:
(see supplementary calculations below coloured hospital maps)
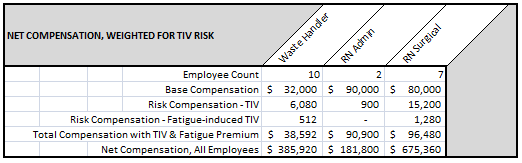
In a traditional payout, the RN Administrator might have highest pay, derived from:
- Years of Service
- Seniority
- Assumed accumulated technical expertise
- Assumed accumulated humane-contact expertise
- Terms of a Collective Agreement
In this model, the RN Surgery Nurse is deemed to be likely to face higher risk of becoming a TI Vector. Therefore, to protect the continuing presence of this person as a public resource, s/he is:
- Deemed to require higher compensation for the risk.
- Able to choose career paths using the Risk/Compensation ratio [ R/C ].
- Able to pre-select or accept shift assignments shifts using R/C Ratio guidelines.
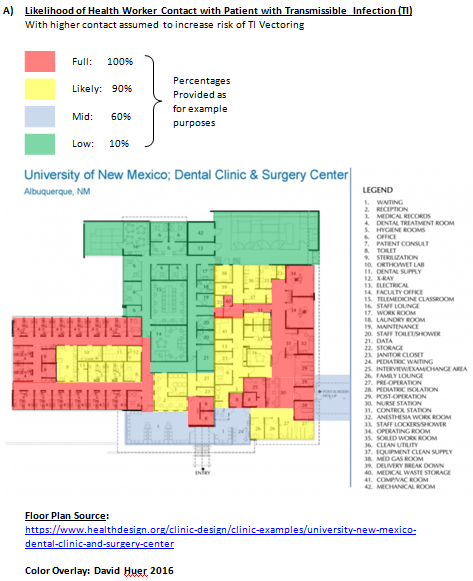
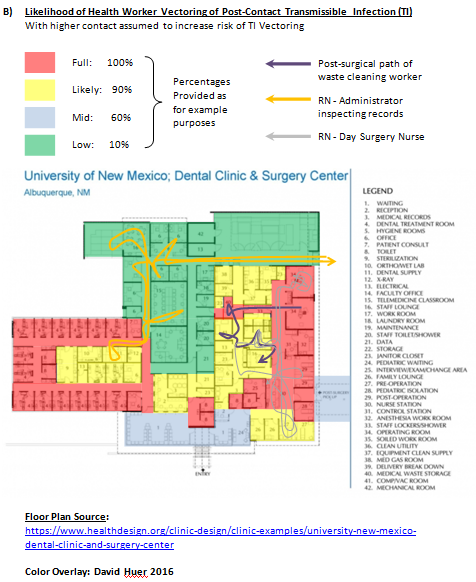
The implications are interesting:
- Health workers of all types (nurses, physicians, security guards, waste cleaning workers, nurse practitioners, administrative staff, mechanical engineers, etc.) experience different levels of stress – and each person’s ability to manage their exhaustion, to obtain compensation, can be hugely challenging. As are suicide and trauma experienced from patient violence and administrative overload. Could TIV-adjusted $compensation packages bring about a new harmoniousness of purpose among health facility staff?
- Could WiFi/GPS/Machine-learning be used to calculate a fluctuating Premium that adjusts to the ability of RNs carrying out their duties?
- Could a higher status Surgeon Emeritus (SE) get lower compensation relative to an Active Surgeon (AS) when the SE faces lower daily risk?
- Could $Premium compensation go up during a full moon or after a sports match? Will workers choose to pick that busy shift knowing the R/C compensation rate?
- Would unexpected source-points and source paths be discovered? For example, the handling path for medical waste held as evidence by a police constable?
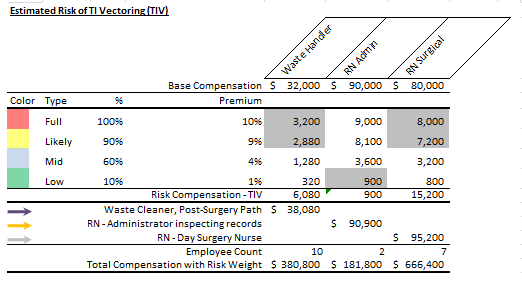
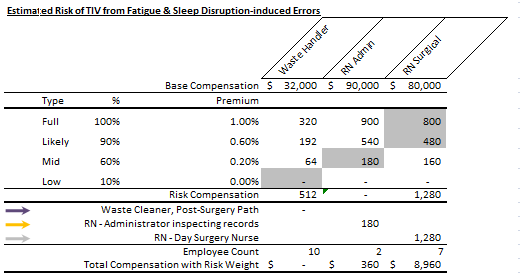
Image:
Students assisting surgery in an affiliated hospital of Hebei North University. https://commons.wikimedia.org/wiki/File:Students_assisting_surgery.JPG, Author: CMSRC, 1 April 2008, 21:27:07, Attribution-ShareAlike 3.0 Unported (CC BY-SA 3.0).
